Reducing Critical Hypoglycemia Through Quality Improvement Initiatives and Implementation of an eGlycemic Management System
Presentation
IHI National Forum on Quality Improvement in Health Care
Date
December 2019
Authors
Debra Dudley,1 Gam Narapanya,2 Michael Yurso,2 Mary Gaines,3 Jennifer Crowe,3
AIM
Reduce critical hypoglycemia (blood glucose <40 mg/dL) among hospitalized patients within two years.
BACKGROUND
On average, one of every three hospitalized patients requires insulin therapy to control blood glucose during their stay, which places them at risk of hypoglycemia. Evidence shows hypoglycemia can lead to infections and other complications, prolonged lengths of stay, increased readmission rates and sentinel events. Preventing hypoglycemia is imperative to patient safety and quality of care. AdventHealth Waterman, a 269-bed community hospital in central Florida, performed a review of all-cause inpatient hypoglycemic events using data over a one-year period, April 1, 2016 – March 31, 2017. The results indicated an opportunity to implement clinical practice changes and other strategies to reduce critical hypoglycemia.
| Patient Population Characteristics | Pre-Intervention | Post-Intervention | p value |
|---|---|---|---|
| Female | 50.3% | 46.6% | — |
| Male | 49.7% | 53.4% | — |
| Total # Patients | 4,615 | 4,104 | — |
| Total # Patient Days (PDs) | 27,475 | 22,970 | — |
| % PDs BG <40 mg/dL | 0.65% | 0.54% | 0.09 |
| % PDs BG <70 mg/dL | 6.19% | 5.74% | 0.04 |
| % PDs BG >300 mg/dL | 7.69% | 9.83% | 0.00 |
| % PDs Avg BG 70-180 mg/dL | 77.5% | 71.39% | 0.00 |
| Critical Hypoglycemic Patient Days <40 mg/dL: Root Cause | Pre-Intervention | Post-Intervention |
|---|---|---|
| Total # Patient Days: All-Cause | 225 | 147 |
| Total # Patient Days: Non-Preventable | 72 | 90 |
| Total # Patient Days: Preventable | 153 | 57 |
METHODS
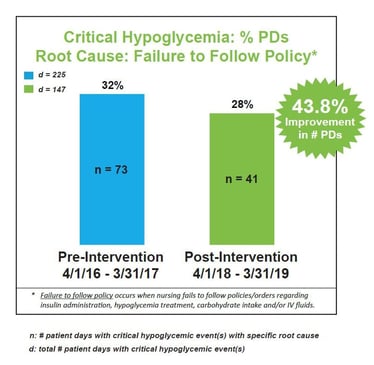
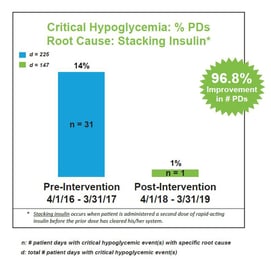
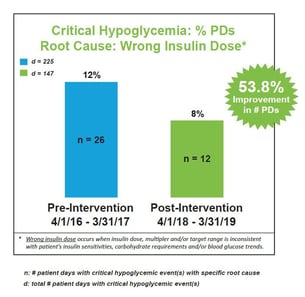
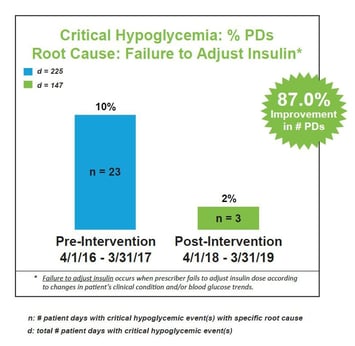
We conducted standardized root cause analysis on all blood glucose values <40 mg/dL. Results identified four areas for targeted interventions: (1) failure to follow policy, (2) stacking insulin, (3) wrong insulin dose, and (4) failure to adjust insulin. An interdisciplinary team was tasked with designing and implementing appropriate clinical practice changes and quality improvement initiatives.
ACTIONS
Education
- Jan 2017 – Diabetes education for nursing champions.
- Oct 2017 – eGlycemic Management System® training for providers and nurses.
- Nov 2017 – Diabetes and insulin education for nurses.
- Feb 2018 – Carb counting education for nurses.
Accountability
- May 2017 – Implementation of hypoglycemia audit tool.
- Nov 2017 – Review of provider and nursing opportunities by leadership.
- Nov 2017 – Development of structured accountability model for providers & nurses.
Workflow & Policies
- Dec 2017 – Go live of eGlycemic Management System® for IV & SubQ insulin dosing.
- Dec 2017 – Update of insulin management policies.
- Mar 2018 – Implementation of carb counting on menus.
CONCLUSIONS
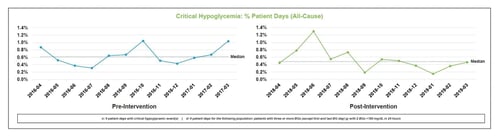
A comparison of pre-intervention data (April 1, 2016 – March 31, 2017) to post-intervention data (April 1, 2018 – March 31, 2019) revealed we reduced all-cause critical hypoglycemia <40 mg/dL by 16.9% of patient days (from 0.65% to 0.54%). The most significant improvements were associated with four areas of targeted interventions: (1) failure to follow policy, (2) stacking insulin, (3) wrong insulin dose, and (4) failure to adjust insulin. We attribute our success to clinical practice changes and quality improvement initiatives coupled with the implementation of a technology-enabled approach to intravenous infusion and subcutaneous basal-bolus insulin dosing using an eGlycemic Management System®.
We recommend that any hospital seeking to achieve best practice and clinical excellence in glycemic management perform a similar root cause analysis of critical hypoglycemic events, define the most appropriate targeted interventions, and utilize education, accountability, workflow and policy measures to achieve their goals.
AFFILIATIONS
- AdventHealth Waterman, Tavares, FL
- AdventHealth Corporate, Altamonte Springs, FL
- Glytec, Waltham, MA and Greenville, SC