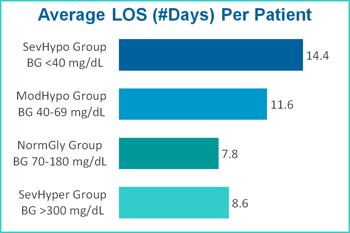Presentation
IHI Annual National Forum on Quality Improvement in Health Care
Date
December 2018
Authors
Mary Gaines, Damon Tanton, Richard Pratley
BACKGROUND
Approximately one-third of all hospitalized patients have diabetes, prediabetes or hyperglycemia. Numerous studies have observed that patients with poor glucose control have longer hospital stays, higher mortality risk and more frequent readmissions.
The Centers for Medicare and Medicaid Services (CMS) penalizes health care institutions for excessive readmissions and mortality rates. Furthermore, CMS is currently (in 2018) considering a severe hypoglycemia “hospital harm” quality measure.
As fee-for-value replaces fee-for-service, health care systems face tremendous pressure to reduce the cost of care associated with complications and longer lengths of stay. The clinical impact of poor glucose control in the hospitalized patient is well established, but a better understanding of the financial impact is needed.
AIM
Identify financial impact of poor glucose control in the hospitalized patient and develop focused glycemic management improvement strategies.
METHODS
The diabetes leadership team at Florida Hospital System evaluated the prevalence and risk of hypoglycemia and hyperglycemia, comparing glucose data to national benchmarks. Point-of-care blood glucose (BG) data was classified into four groups:
| Group | Definition | Blood Glucose Value | Number/Percent of Patients |
|---|---|---|---|
| SevHypo Group | Severe Hypoglycemia | <40 mg/dL | 742 (1.7%) |
| ModHypo Group | Moderate Hypoglycemia | 40-69 mg/dL | 6,985 (16.0%) |
| NormGly Group | Normal Glycemia | 70-180 mg/dL | 24,885 (57.0%) |
| SevHyper Group | Severe Hyperglycemia | >300 mg/dL | 11,047 (25.3%) |
Correlations between BG data and mortality rates, lengths of stay, readmissions and hospital costs were analyzed for each group. Focused improvement strategies were designed and implemented using the Plan-Do-Study-Act model targeting the group shown to have the highest clinical and financial risks.
RESULTS
Analysis of data from 43,659 patients admitted to seven hospitals in the Florida Hospital System over a 12-month period in 2015-16 showed those in all groups other than the Normal Glycemia group had higher mortality rates, longer hospital stays, more frequent readmissions and significantly greater costs. Most notably, patients in the Severe Hypoglycemia group were observed to have the highest risks across all measures.
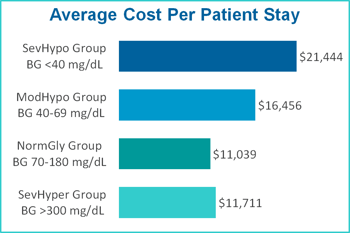
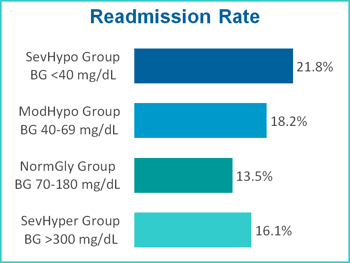
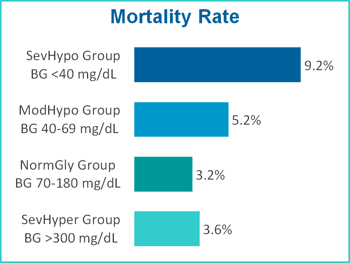
Incidence of severe hypoglycemia was observed to have a significant impact on financial outcomes, increasing the total cost of care by nearly $7.7 million over the 12-month period. Patients in the Severe Hypoglycemia group incurred an average cost per stay $10,405 higher than patients in the Normal Glycemia group. The Severe Hypoglycemia group also had a higher readmission rate (by 61.5%), a longer average length of stay (by 6.6 days) and a mortality rate nearly three times more compared to the Normal Glycemia group.
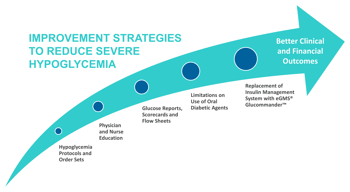
Armed with this information, Florida Hospital System developed strategies to reduce the impact and frequency of severe hypoglycemia. The planned interventions were implemented over several years with modification to each of the initiatives after studying the respective results.
| Group | Average Cost Per Patient Stay | Average LOS (#Days) Per Patient | Readmission Rate | Mortality Rate |
| SevHypo Group | $21,444 | 14.4 | 21.8% | 9.2% |
| ModHypo Group | $16,456 | 11.6 | 18.2% | 5.2% |
| NormGly Group | $11,039 | 7.8 | 13.5% | 3.2% |
| SevHyper Group | $11,711 | 8.6 | 16.1% | 3.6% |
CONCLUSIONS
An in-depth analysis of data across Florida Hospital System revealed that poor glucose control has a significant impact on mortality, length of stay, readmissions and costs. The results highlight that strategies to reduce incidence of hypoglycemia and hyperglycemia are imperative to patient safety and quality of care as well as sustained clinical and operational excellence.
It is recommended that all health care systems undertake a similar process to identify at-risk populations and formulate targeted improvement strategies. Failure of health care systems to recognize the impact of poor glucose control and to invest in resources and technologies for optimizing glycemic management will result in substantial financial penalties, excess cost and revenue loss.