eGlycemic Management System®
Revolutionizing glycemic management by uniting teams around patient safety.
Introduction
eGlycemic Management System (eGMS) is an EHR-integrated, cloud-based software solution that supports safe and effective glycemic management and insulin dosing.
eGMS offers personalized insulin dosing decision support at the point of care. Unlike paper protocols, sliding scale methods and digital insulin calculators, eGMS optimizes insulin therapy with Glucommander®, evidence-based, FDA-cleared software. Glucommander leverages real-time and historical data to personalize insulin dosing by learning each patient’s insulin sensitivity and anticipating future need.
The result? Patients experiencing glycemic management challenges get into target range faster [1], stay within tighter parameters [2] and experience fewer insulin-related adverse drug events [3] than patients treated with other protocols.
In addition to dosing support, eGMS offers tools for doctors, nurses, pharmacists, CDCESs, hospital leadership and others to optimize glycemic management. These tools include:
- Advanced glycemic management analytics
- Continuous surveillance of blood glucose levels across the entire patient population
- Dynamically adjusted timing for BG checks with automated reminders
- Dashboards to support coordination of care
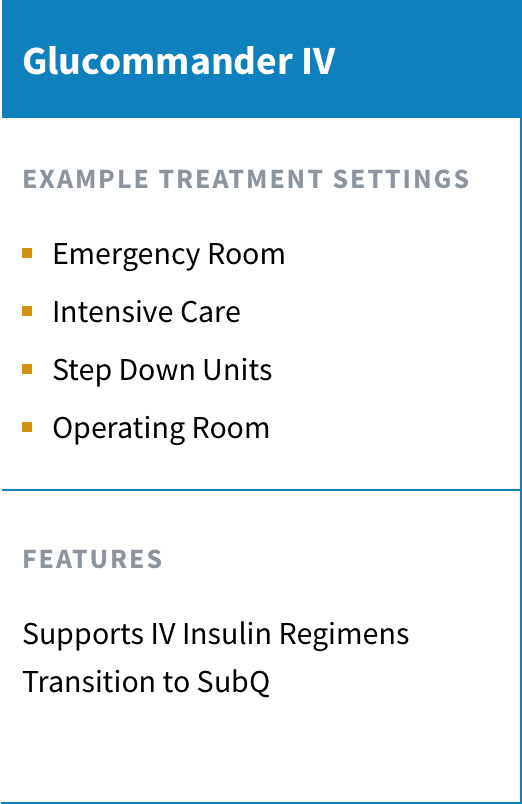
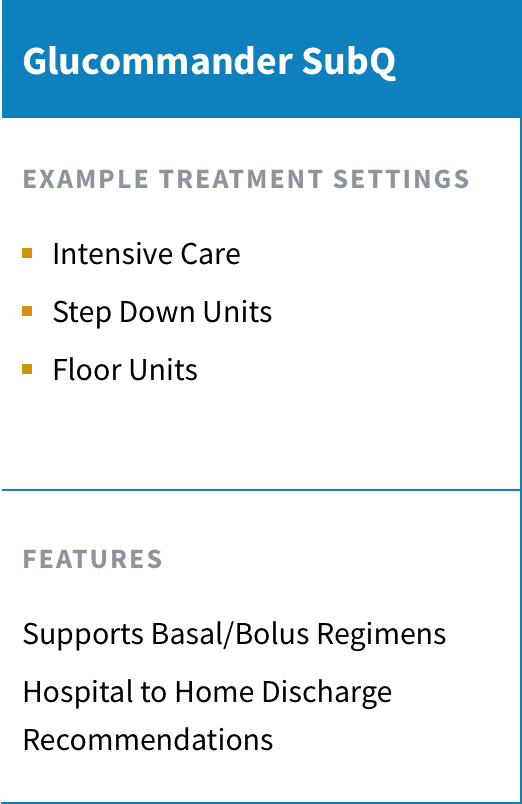
Glucommander provides insulin dosing decision support and is FDA-cleared for use with adult and pediatric patients ages 2 and above. Glucommander is available in 3 different treatment modules that support patients and providers across the continuum of care.
Healthcare facilities can decide to implement one or more Glucommander treatment modules based on the units and care settings at their facilities:
Glucommander Treatment Modules
|
INPATIENT CARE |
|
OUTPATIENT CARE |
|
Includes the full suite of eGMS Modules to support insulin dosing support: |
Watch the Product Overview Video:
Glycemic Management Status Quo
The glycemic management status quo is unsustainable
Insulin dosing in the inpatient setting has remained largely unchanged for half a century. Simplified protocols seek to ease provider burden but can’t provide personalized care. Meanwhile, more complex protocols that are dependent on manual calculations are prone to dangerous errors.
What these status quo methodologies have in common is that they’re not safe and they’re not the standard of care.[4]
Sliding scale and other one-size-fits-all protocols are outdated and dangerous, resulting in higher rates of hyperglycemia and hypoglycemia than Glytec’s personalized, algorithm- driven solution. [2] Reliance on protocols that don’t dynamically adjust based on patient needs is strongly discouraged by the American Diabetes Association. [4]
In addition, traditional paper protocols and most digital insulin dosing calculators provide no data for further analysis and lack safety guardrails to prevent errors in treatment.
Considered alongside the increasing prevalence of diabetes in the U.S. [3] and the outsized impact [5][6] patients with glycemic issues have on the healthcare system, reliance on the status quo is a recipe for disaster.
And it’s not just people with diabetes who require insulin in the hospital; stress hyperglycemia is often found with patients who are undergoing surgery or who are critically ill[7]. These patients are often not given insulin therapy that has been proven to improve their outcomes because status quo methodologies don’t have a way of identifying them.
Glycemic management in the U.S.:
|
1 in 3Americans has glycemic control issues (diabetes or prediabetes) [5] |
38%Of inpatients require insulin therapy during their hospital stay [7] |

2.3xAmericans with diabetes have 2.3x greater health care costs than those without [6] |
16.3%Insulin is involved in 16.3% of medication errors reports for high-alert medications, more than any other medication type. [8] |
Glycemic Management Reimagined
Glycemic management reimagined
Ineffective glycemic management has consequences that reach far beyond the patient bed, and stakeholders throughout the hospital have a role to play in ensuring the safe and effective treatment of patients with glycemic issues.
eGMS is a holistic solution for improving glycemic management throughout the healthcare system. Our cloud-based, EHR-integrated technology unites doctors, nurses, pharmacists, quality teams, hospital leadership and others around a common goal: better, safer care.
By equipping all stakeholders with the tools and data they need to make better decisions, eGMS has been repeatedly proven to enhance patient safety, improve quality of care and decrease costs compared to the status quo.
Real results from real hospitals:
|
99.8% reduction in frequency of severe hypoglycemia [9] |
3.2 days reduction in average length of stay [2] |
36-68% reduction in 30-day readmissions for AMI, CHF and CABG patients [10] |
|
62.6% reduction in preventable hypoglycemia-related adverse drug events [3] |
$2,934 saved per hypoglycemic event prevented [2] |
Up to 72 minutes per nurse per patient saved for patients using IV insulin [12] |
Glucommander
Glucommander: Insulin dosing decision support
Our algorithm-driven insulin dosing software is the heart of eGMS. Glucommander is FDA-cleared and indicated for use in IV, SubQ and outpatient settings.
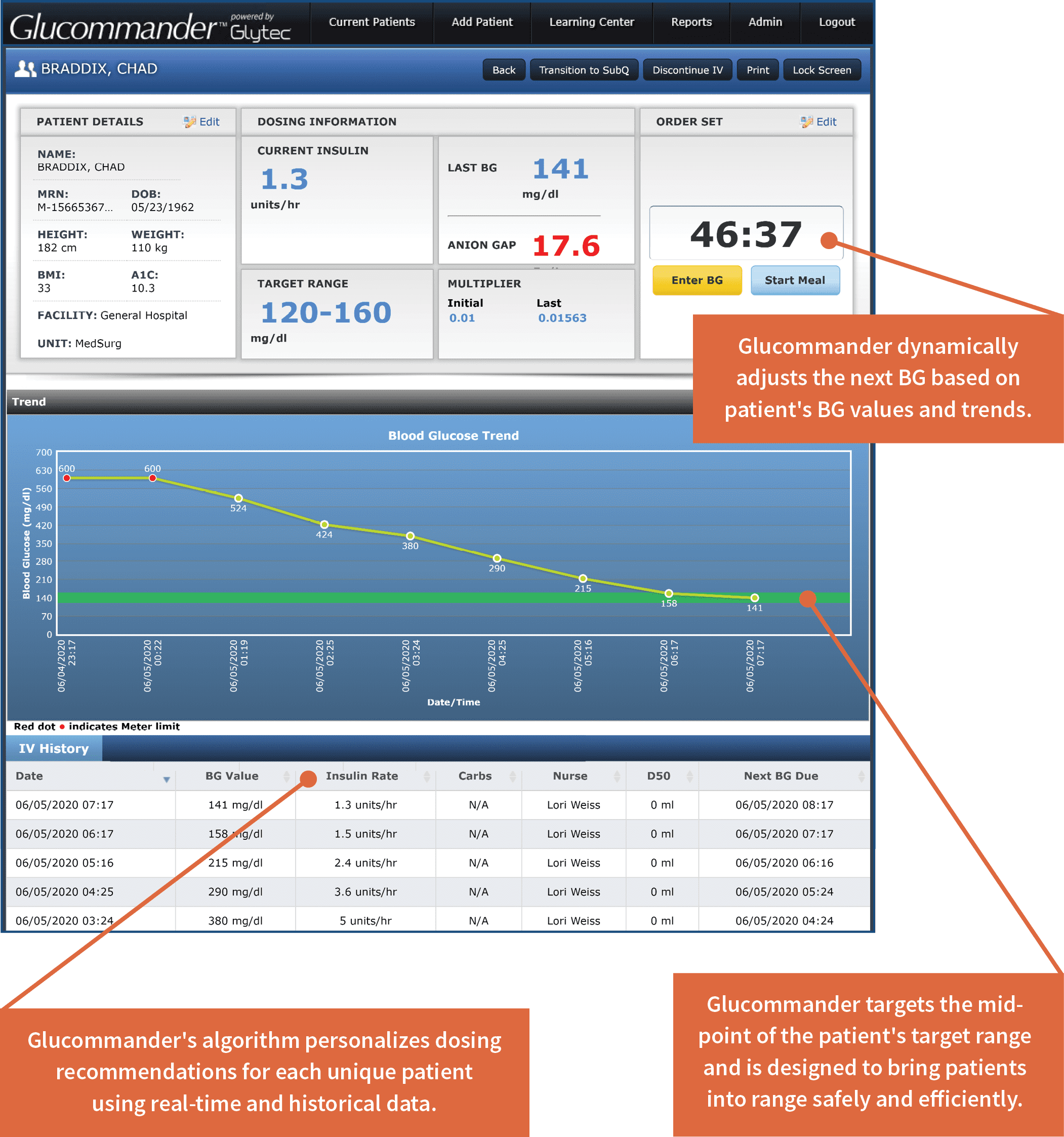
Glucommander: IV Workflow example

Safety Guardrails
Safety guardrails
Glucommander includes an array of safety features to guide best practice insulin dosing methodology and improve patient safety and outcomes. These guardrails supplement clinicians’ decision-making by leveraging available data to draw their attention to potentially dangerous situations.
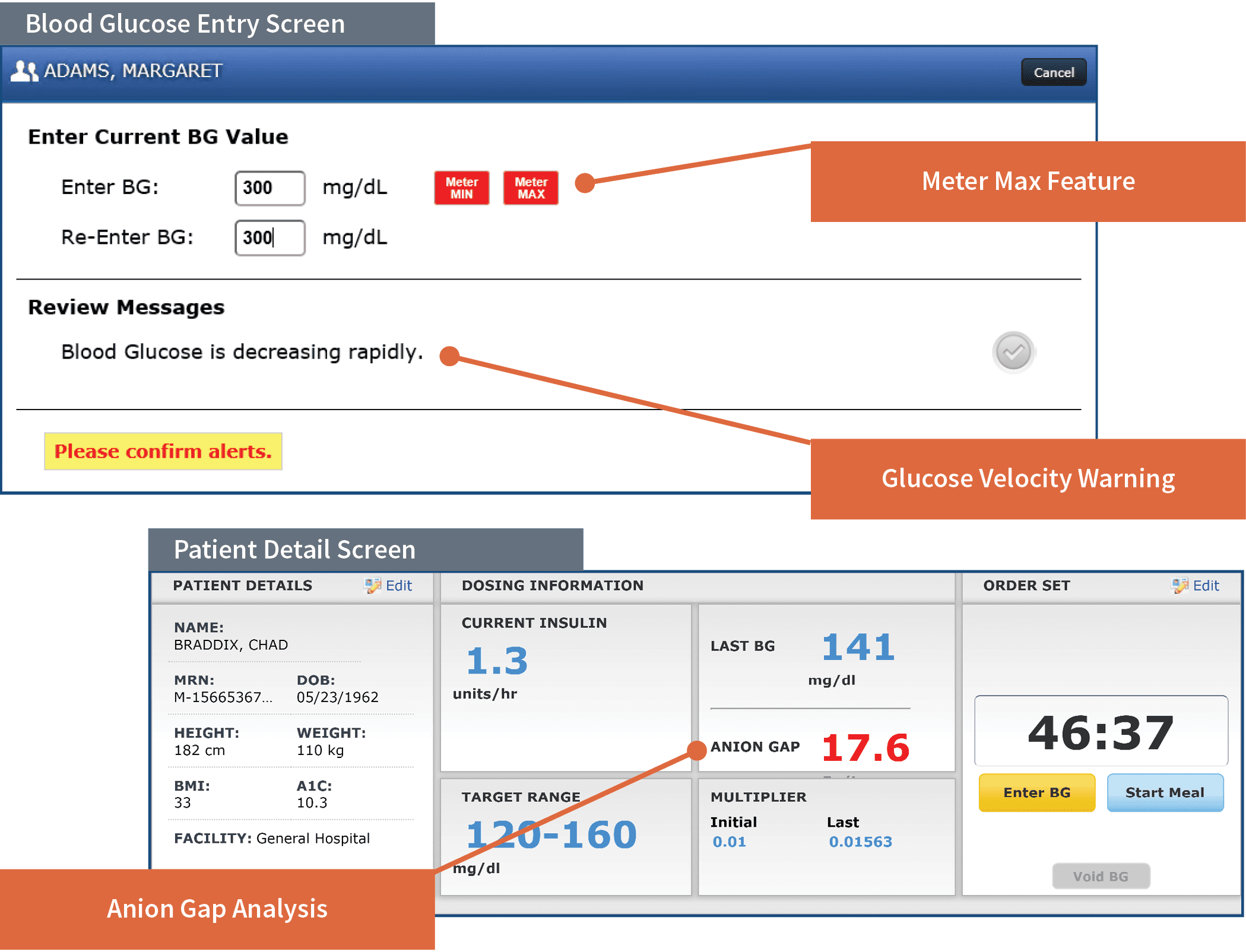
- Glucose velocity warning: Alerts nurses about sudden drops in patient blood glucose and prompts a BG recheck sooner to ensure that patients achieve target range safely. This feature is designed to prevent hypoglycemia and side effects like cerebral edema that are caused by rapid decrease in blood glucose.
- Anion gap analysis: Alerts nurses to high anion gaps to prevent premature discontinuation of treatment before resolution of DKA.
- Meter Max™ feature: Allows nurses to leverage the algorithm’s ability to recommend insulin doses when blood glucose values are above the glucose meter limit without waiting for lab values. Designed to prevent large drops in BG values so the patient achieves target range as soon as safely possible.
Integrations and Access
Integrations & Access
Accurate data is critical to calculating a personalized, safe and effective insulin dose. Glytec's HITRUST certified platform utilizes secure integrations with health systems’ EHRs to capture relevant data that already exists and to close the data loop with minimal data entry, which improves patient safety and reduces workflow friction for clinicians.
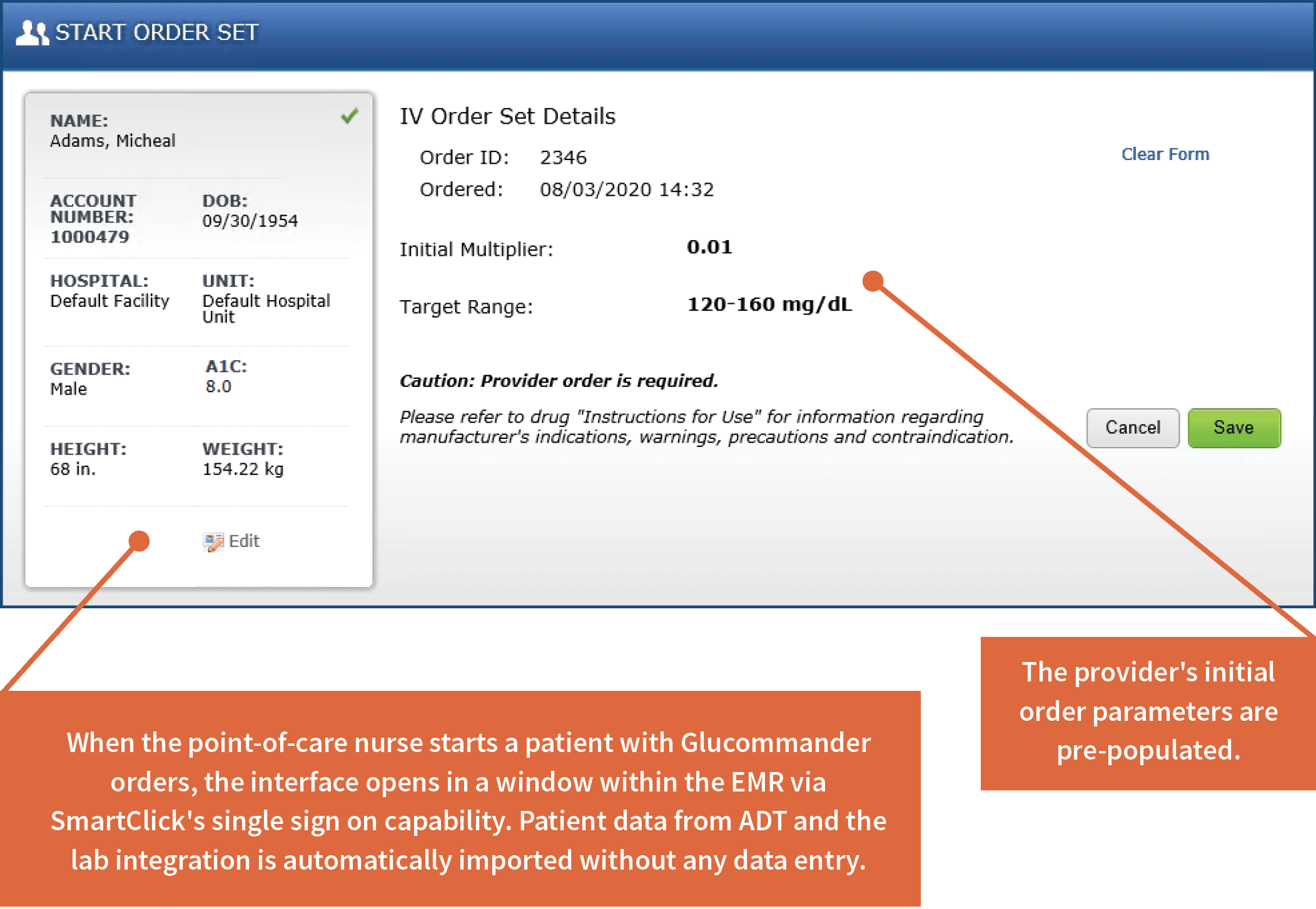
- SmartClick: Enables single sign-on and access to eGMS from within the EHR
- ADT: Imports patient information like demographics, height and weight
- Lab Results: Imports lab results like A1C, blood glucose and anion gap
- Order: Glucommander automatically receives initial parameters as ordered by the provider and displays this information when the nurse starts treatment
- Charting: Charts Glucommander data on the EHR flowsheet to display all patient care history in a single location without needing to double document
- Medication administration confirmation: Once a medication is charted on the MAR, the interface sends dose confirmation back to Glucommander to close the data loop without manual effort
GlucoView
GlucoView®: Glycemic status and alerts
eGMS includes a dashboard of glycemic status indicators for all patients in a unit, supporting team nursing and coordination of care (especially during shift changes).
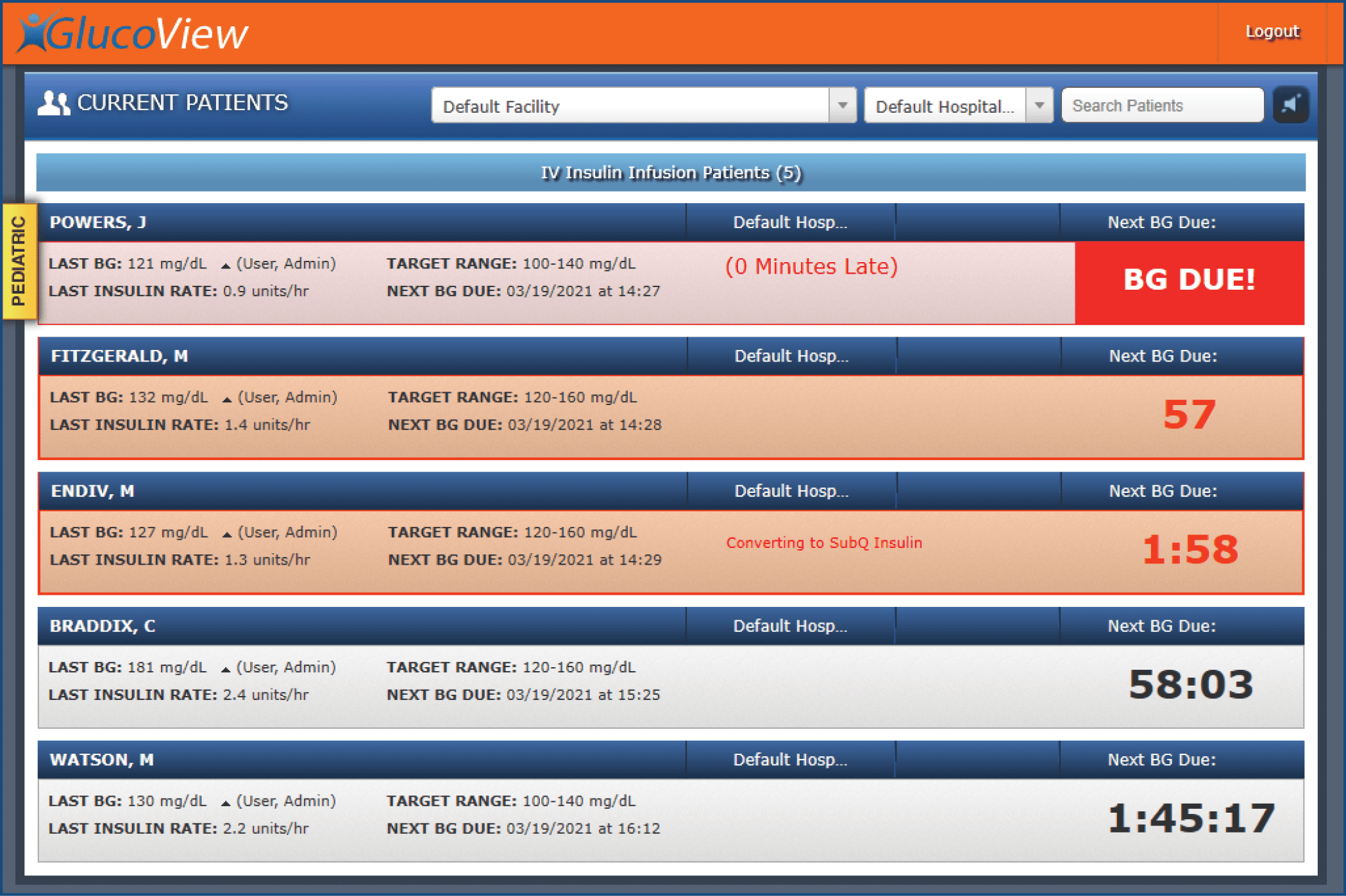
|
GlucoView allows nursing teams to see Next BG Due for all patients in one view, so they can proactively plan and prioritize patient care. |
GlucoSurveillance
GlucoSurveillance®: At-risk patient identification
eGMS interfaces with the hospital’s laboratory information system to continuously analyze the blood glucose values of all patients for whom data is available (not just those with Glucommander orders) to proactively identify patients with hyperglycemia.
The GlucoSurveillance dashboard notifies the designated clinician about patients with hyperglycemia who are at risk for adverse effects. Using GlucoSurveillance, providers can treat patients needing insulin therapy sooner, which improves patient safety.
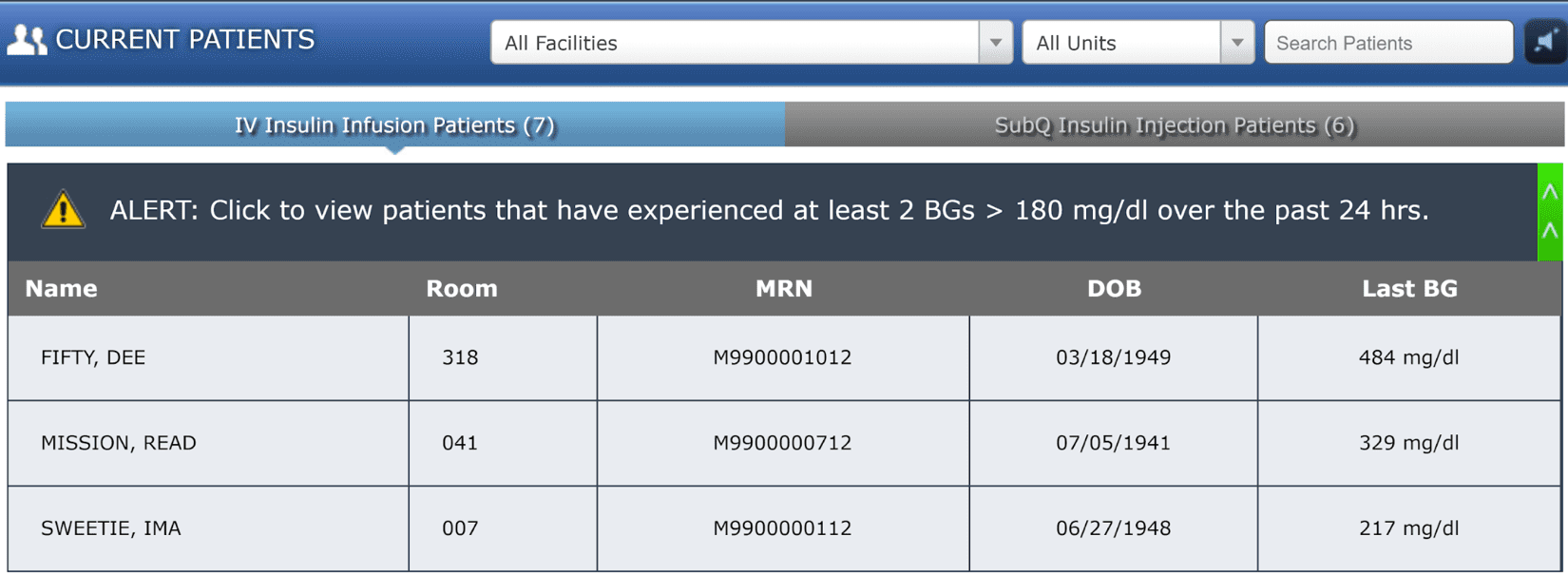
| GlucoSurveillance can be used by individual providers to monitor their patients, but is also a tool used by CDCES teams or designated clinical leads to identify and recommend treatment. |
GlucoMetrics and Reports
GlucoMetrics®: Glucose data analytics and reporting
GlucoMetrics and Glytec’s other reporting capabilities give providers, nurses, glycemic management committees, and executive leadership 24/7/365 self-serve access to the outcome and process metrics that matter most to them. And it’s easy.
GlucoMetrics comes complete with pre-configured dashboards that make analytics such as incidence of hyperglycemia and hypoglycemia easy to track, internal benchmarks easy to set, and quality improvement (QI) projects easy to start. And our team is with you every step of the way.
Working with your Clinical Customer Success Manager, you can customize your dashboards to show your favorite views, learn how to share them easily across your teams, and create email subscriptions so key insights are always top of mind.
System-Level Metrics
View glucose management analytics from across the healthcare system in one location as measures of either blood glucose value, patient day, or patient stay.
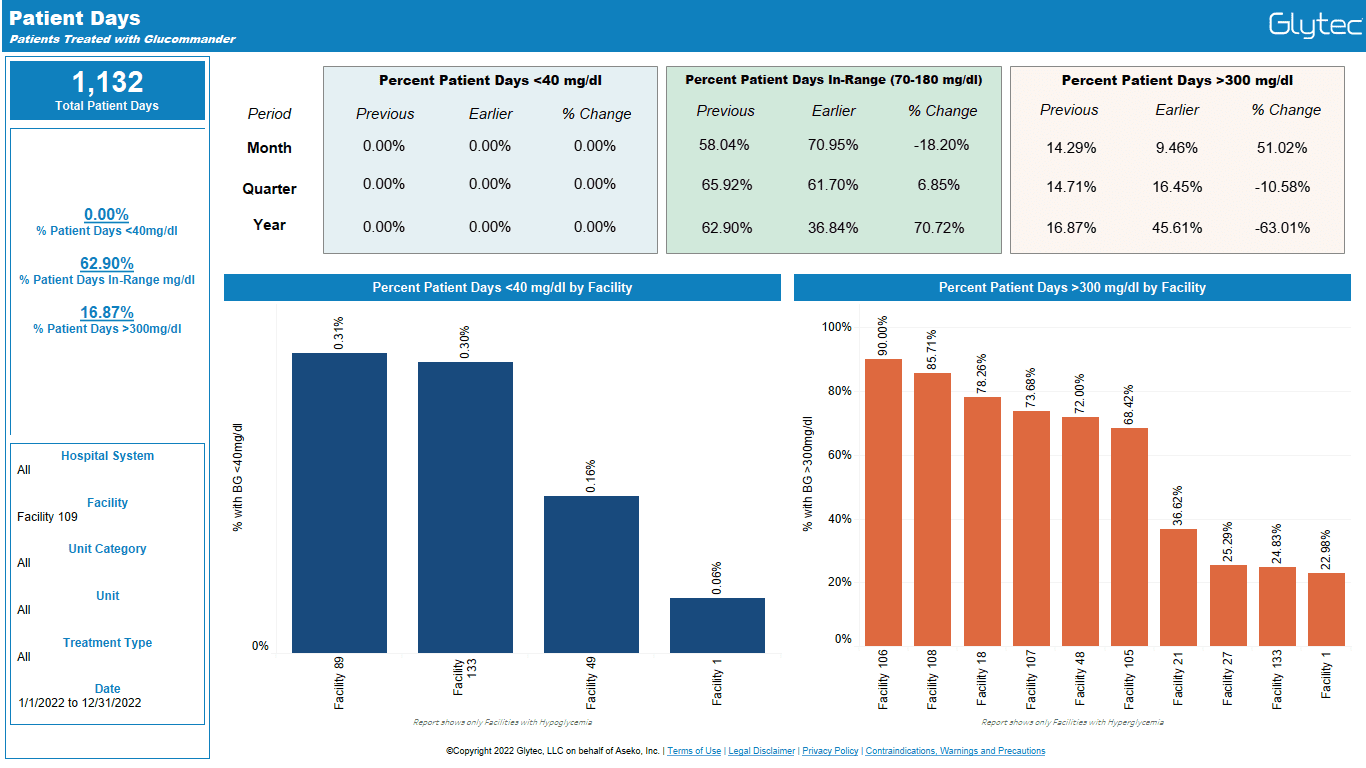
Filters allow you to easily compare based on any combination of time period, treatment type, facility, unit category, and unit.
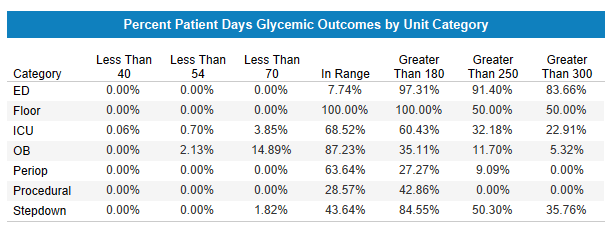
Dynamic Data Visualizations Bring Key Analytics Into Focus
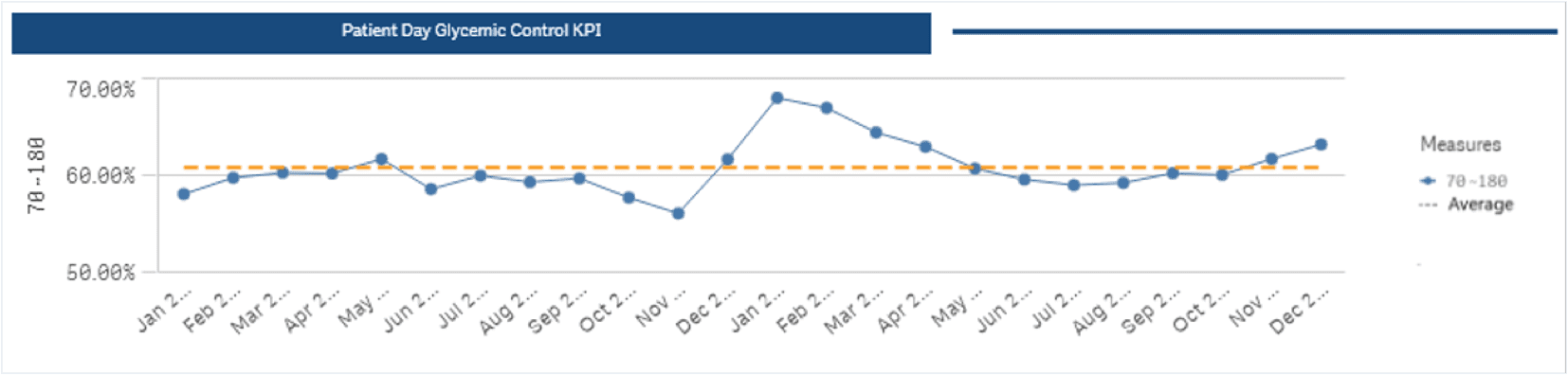
View hypoglycemia and hyperglycemia as balancing measures in one chart, track in-range percentages over time, and immediately see where instances of severe hypoglycemia and hyperglycemia are occurring without needing to configure reports or manage spreadsheets.
Track Adherence to Glycemic Management Best Practices
The Blood Glucose Check Timeliness dashboard shows which facilities, units and unit categories are most often checking Glucommander IV patients within the recommended 10 minutes of the time BGs are due, and the Treated vs. Untreated dashboard compares outcomes of patients on Glucommander vs those with persistent hyperglycemia who aren’t.
Implementation and Support
A proven process for change management
Glytec’s streamlined post-purchase process ensures all stakeholders have exactly what they need to achieve great results. Our cloud-based technology enables remote implementation and upgrades and reduces reliance on your technical resources to maintain the software. Glytec is the only insulin dosing decision support provider that is HITRUST certified, reflecting our ability to meet the highest standards for protecting healthcare partners' sensitive data and information.
Highlights:

Quick turnaround (as little as 8 weeks) |

100% remote implementation and update capabilities |

Standardized technical process to minimize IT lift and provide assistance and resources for implementation |

Training modules and resources delivered via your own e-learning system |

Unlimited 24/7/365 clinical and technical support |

No additional cost for training and support |
| Implement in as little as 8 weeks. |
eGMS is EHR agnostic - we’ve completed hundreds of implementations that integrate with Epic and Cerner, as well as many other EHR platforms. Our team can provide more details about integrating with your specific EHR during a consultation.
Download eGMS Brochure
Download GlucoMetrics Brochure
References
-
Comparative Effectiveness of a Computerized Algorithm Versus a Physician Instituted Protocol to Manage Insulin Infusions After Cardiac Surgery. Clinical Medicine & Research, Apr 2014.
-
Newsom R, Patty C, Camarena E, et al. Safely converting an entire academic medical center from sliding scale to basal bolus insulin via implementation of the EGLYCEMIC Management System. Journal of Diabetes Science and Technology. 2017;12(1):53-59. doi:10.1177/1932296817747619.
-
Dudley D, Gaines M. Use of Technology Reduces Incidence of Hypoglycemia-Related Adverse Drug Events Among Patients Re- quiring Insulin Therapy While Hospitalized. DTS Virtual Poster Meeting. June 18, 2020.
-
15. Diabetes Care in the Hospital: Standards of Medical Care in Diabetes—2020. American Diabetes Association. Diabetes Care Jan 2020, 43 (Supplement 1) S193-S202; DOI: 10.2337/dc20-S015
-
Centers for Disease Control and Prevention. National Diabetes Statistics Report, 2020. Atlanta, GA: Centers for Disease Control and Prevention, US Department of Health and Human Services; 2020. ttps://www.cdc.gov/diabetes/data/statistics/statistics-report.html
-
Economic Costs of Diabetes in the U.S. in 2017. American Diabetes Association. Diabetes Care 2018 Mar; dci180007. https://doi.org/10.2337/dci18-0007
-
Guillermo E. Umpierrez, Scott D. Isaacs, Niloofar Bazargan, Xiangdong You, Leonard M. Thaler, Abbas E. Kitabchi, Hyperglyce- mia: An Independent Marker of In-Hospital Mortality in Patients with Undiagnosed Diabetes, The Journal of Clinical Endocrinol- ogy & Metabolism, Volume 87, Issue 3, 1 March 2002, Pages 978–982, https://doi.org/10.1210/jcem.87.3.8341
-
Pennsylvania Patient Safety Authority. Focus on high-alert medications. Pa Patient Saf Advis. 2004;1(3):6. http://patientsafety.pa.gov/ADVISORIES/Pages/200409_06.aspx
-
Rabinovich, M., Grahl, J., Durr, E., Gayed, R., Chester, K., McFarland, R., & McLean, B. (2018). Risk of Hypoglycemia During Insulin Infusion Directed by Paper Protocol Versus Electronic Glycemic Management System in Critically Ill Patients at a Large Academ- ic Medical Center. Journal of Diabetes Science and Technology, 12(1), 47–52. https://doi.org/10.1177/1932296817747617
-
Mumpower A, Parsons T. Relationship Between Glycemic Control Using eGMS and Readmission Rates in Cardiovascular Patients Hospitalized with AMI, CHF or Undergoing CABG During the Implementation of a System Wide Glycemic Initiative. 1. 2016 Diabe- tes Technology Meeting Abstracts. Journal of Contemporary Ethnography. 2017;11(2):645-668. doi:10.1177/0891241606286997
-
Newsom R, Patty C, Camarena E, Gray T, Sawyer R, Brown B, McFarland R. Safely Converting From Sliding Scale to Basal Bolus Insulin Across an Entire Medical Center via Implementation of the eGlycemic Management System. American Diabetes Association Scientific Sessions. June 2017.
-
Mabrey M, Clark J, Burks J, McFarland R, Hebblewhite H, Williams A. New Interfaces for eGlycemic Management System Saves Nursing Time and Improves Patient Outcomes: Time and Motion Nursing Study. Poster presented at: American Association of Clinical Endocrinologists Scientific & Clinical Congress; May 2014; Las Vegas, Nevada
MAR 0000770 Rev 1.0